Subjective Cognitive Decline by US State: High-Resolution Infographics
Published on October 15, 2025
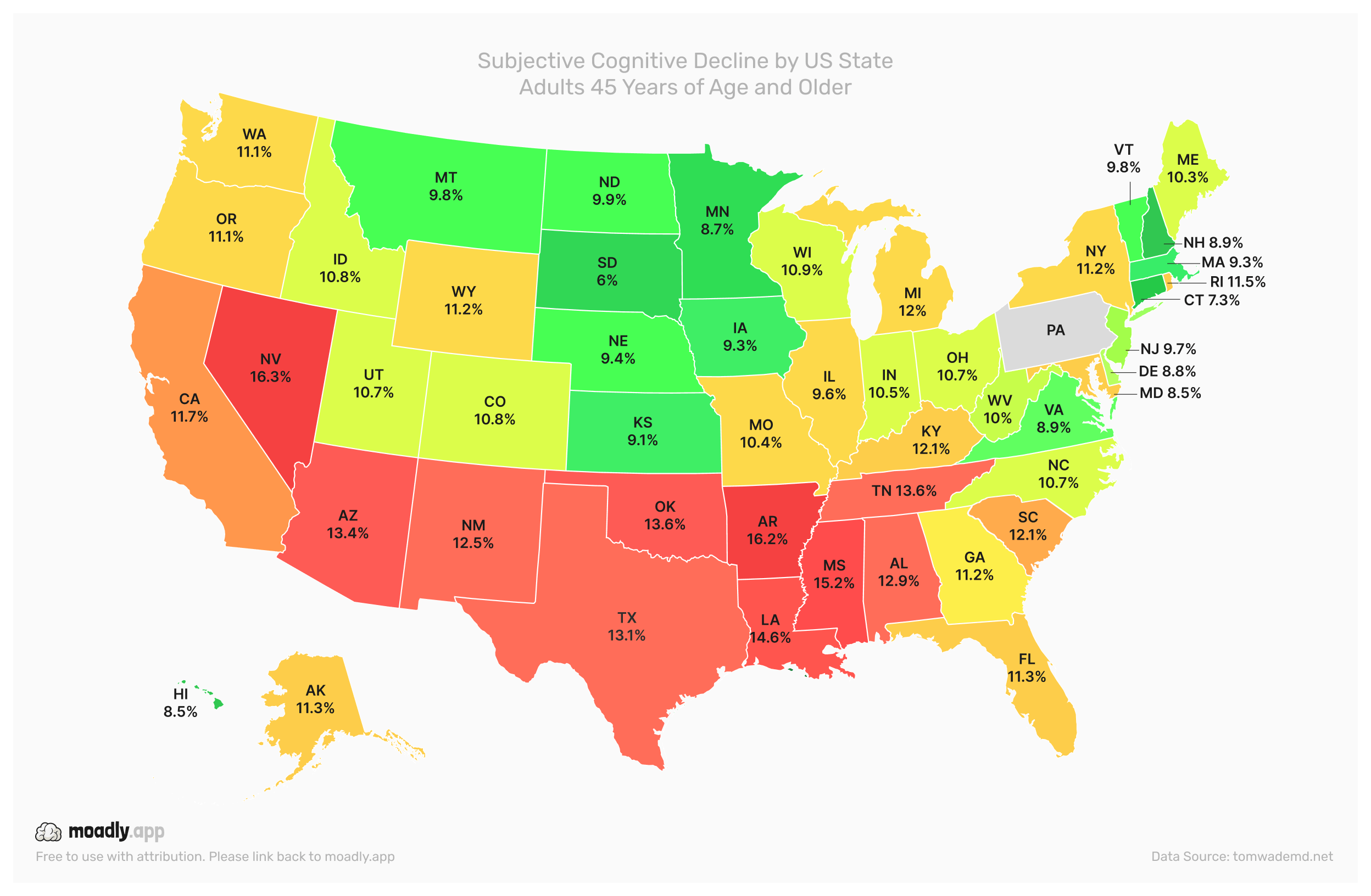
Memory concerns are becoming increasingly common among U.S. adults aged 45 and older. One way researchers track these changes is through Subjective Cognitive Decline (SCD), which refers to self-reported experiences of worsening memory or confusion over the past year. While SCD does not confirm a clinical diagnosis, it can serve as an early indicator of cognitive decline. Understanding its patterns can help highlight regions where public health support may be needed most.
This article draws on data and insights from the CDC-based SCD public health overview compiled by Tom Wade, MD. By referencing this source, we provide an accurate look at national trends in memory concerns among adults aged 45 and older.
The map below shows the prevalence of SCD across the country. States with the lowest reported levels are shaded in green, mid-range levels appear in yellow, and states with the highest prevalence are shown in red. This visual representation makes regional differences in memory concerns immediately apparent.
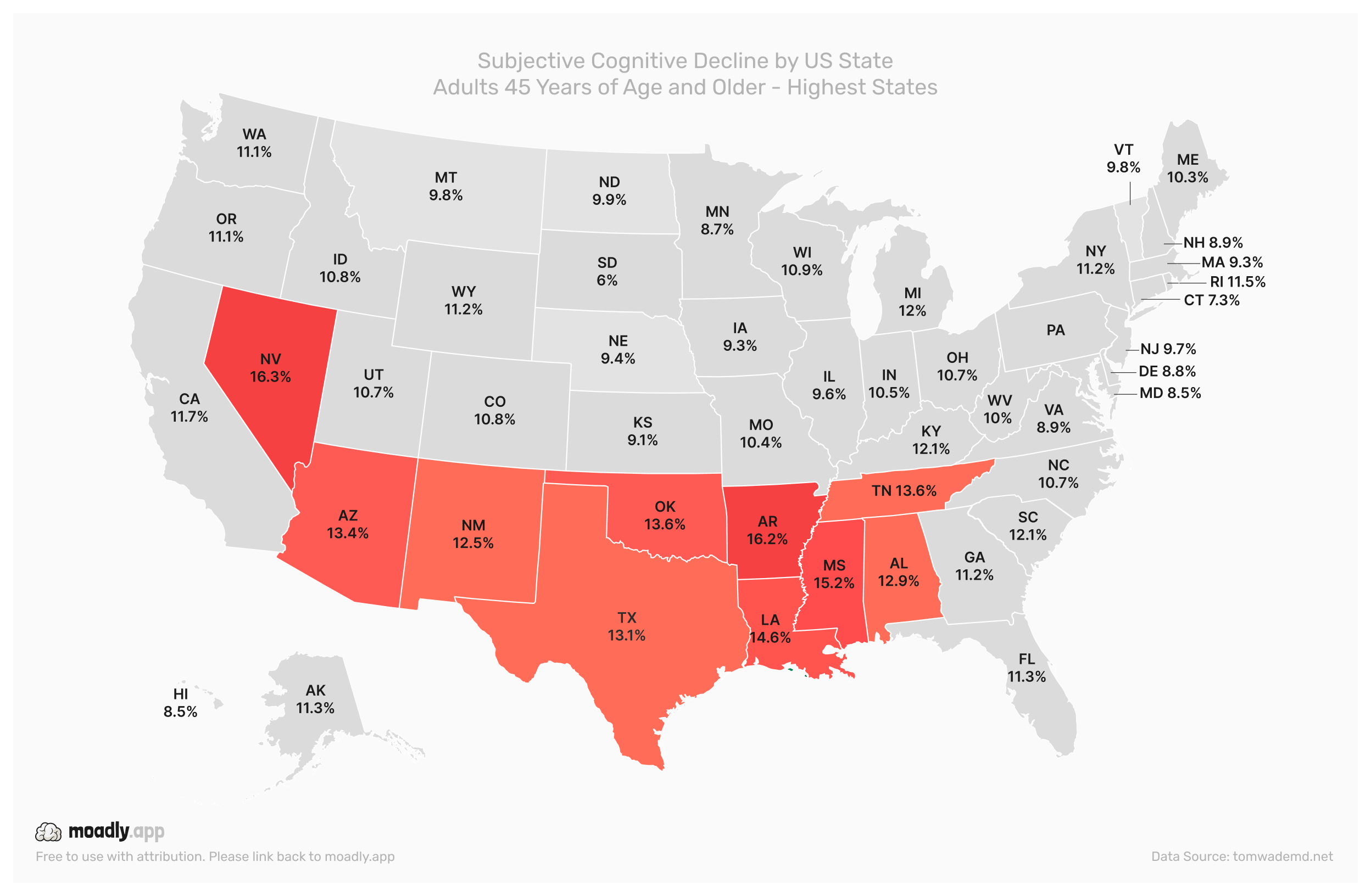
According to the data, the highest prevalence of SCD is concentrated in Southern and Southwestern states, including Nevada, Arizona, New Mexico, Oklahoma, Texas, Arkansas, Mississippi, Louisiana, Alabama, and Tennessee. In these states, a significant portion of adults report increasing memory problems. Socioeconomic factors, limited access to healthcare, differences in education, and community support structures may all contribute to these higher rates.
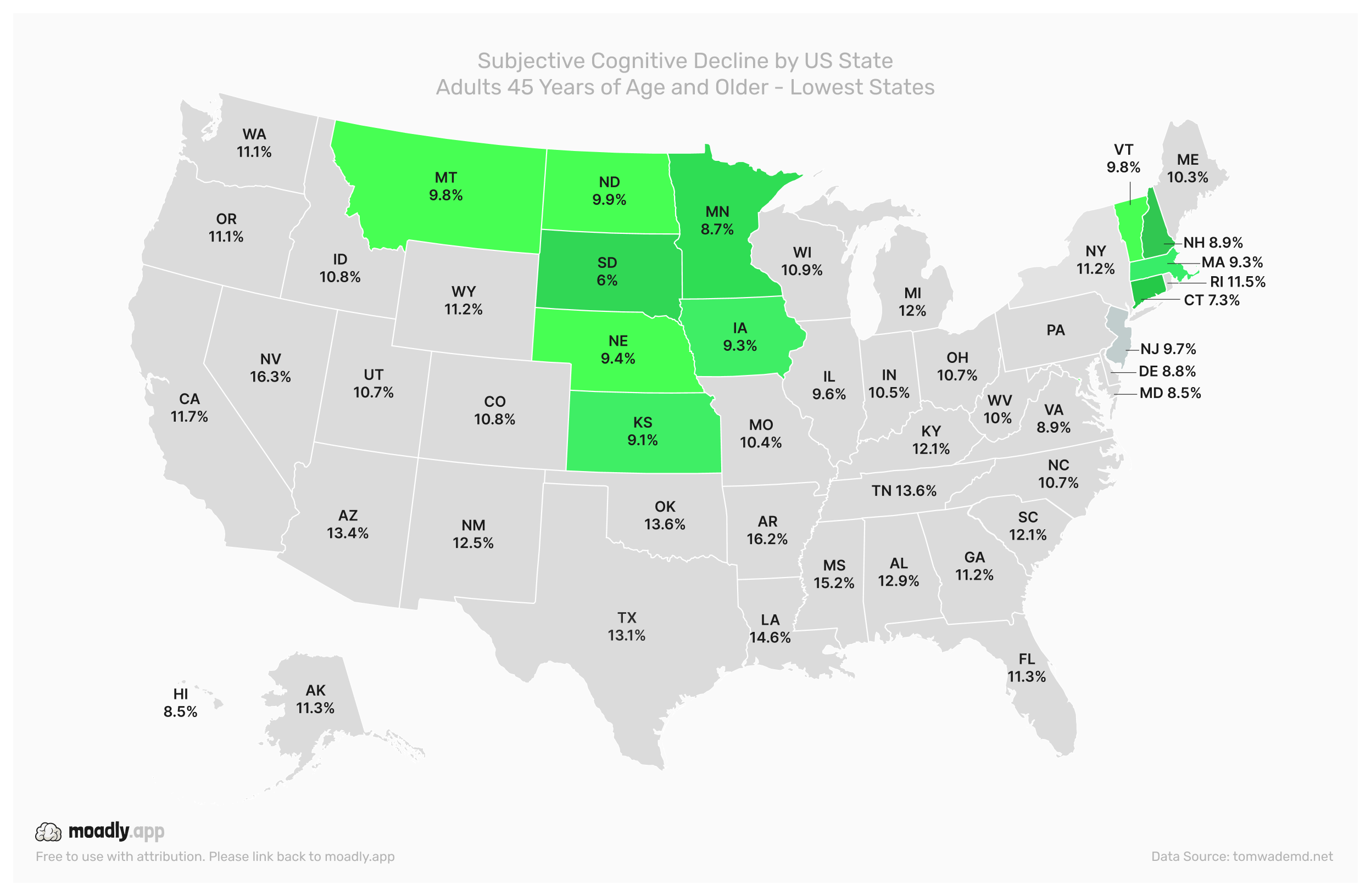
On the other end of the spectrum, the lowest prevalence of SCD is seen in states such as South Dakota, Minnesota, Iowa, New Hampshire, Massachusetts, Connecticut, Montana, and Nebraska. These states report fewer adults experiencing frequent memory issues. Factors such as higher educational attainment, stronger healthcare access, and supportive community environments may help explain these lower rates.
States with mid-range prevalence appear in yellow and orange, showing a gradual variation across the country. This highlights that SCD is not confined to a handful of states-it occurs nationwide to varying degrees. Understanding these patterns can help public health officials focus interventions, allocate resources effectively, and design education and screening programs where they are most needed.
Overall, this map offers a snapshot of cognitive health among U.S. adults aged 45 and older. Recognizing where SCD is most common can guide communities in supporting adults experiencing memory loss, promoting early healthcare engagement, and mitigating the long-term impact of cognitive decline.
Some states report lower rates of Subjective Cognitive Decline (SCD), indicating relatively better cognitive health among adults aged 45 and older. Factors such as higher education levels, better access to healthcare, and supportive community environments may contribute to these differences. Examining these regions can provide insights into strategies for reducing cognitive decline nationwide.
Key Findings
1. Prevalence of Subjective Cognitive Decline
Approximately 11.1% of adults aged 45 and older report experiencing SCD, with slightly higher prevalence among adults aged 65+ (11.7%) compared to those aged 45–64 (10.8%). Prevalence also varies across sex, race/ethnicity, and educational attainment, reflecting demographic and socioeconomic differences in the population.
2. Living Alone and Vulnerability
Nearly 30% of adults with SCD live alone, which may increase vulnerability to health complications, self-neglect, and challenges in managing daily tasks independently. Older adults in particular may face higher risks when living alone.
3. Healthcare Discussion
Fewer than half of adults experiencing SCD have discussed their symptoms with a healthcare professional. This highlights an opportunity for improved screening, earlier intervention, and stronger communication between patients and providers.
4. Coexisting Chronic Conditions
Around two-thirds of adults with SCD also have two or more chronic health conditions. Managing multiple conditions can be more difficult and often increases reliance on caregivers or healthcare services.
5. Mental Distress and Daily Function
Approximately one-third of adults with SCD report frequent mental distress, and more than half experience functional difficulties related to cognitive decline. These challenges can affect daily living, work performance, and social participation.
State-by-State Average IQ Table
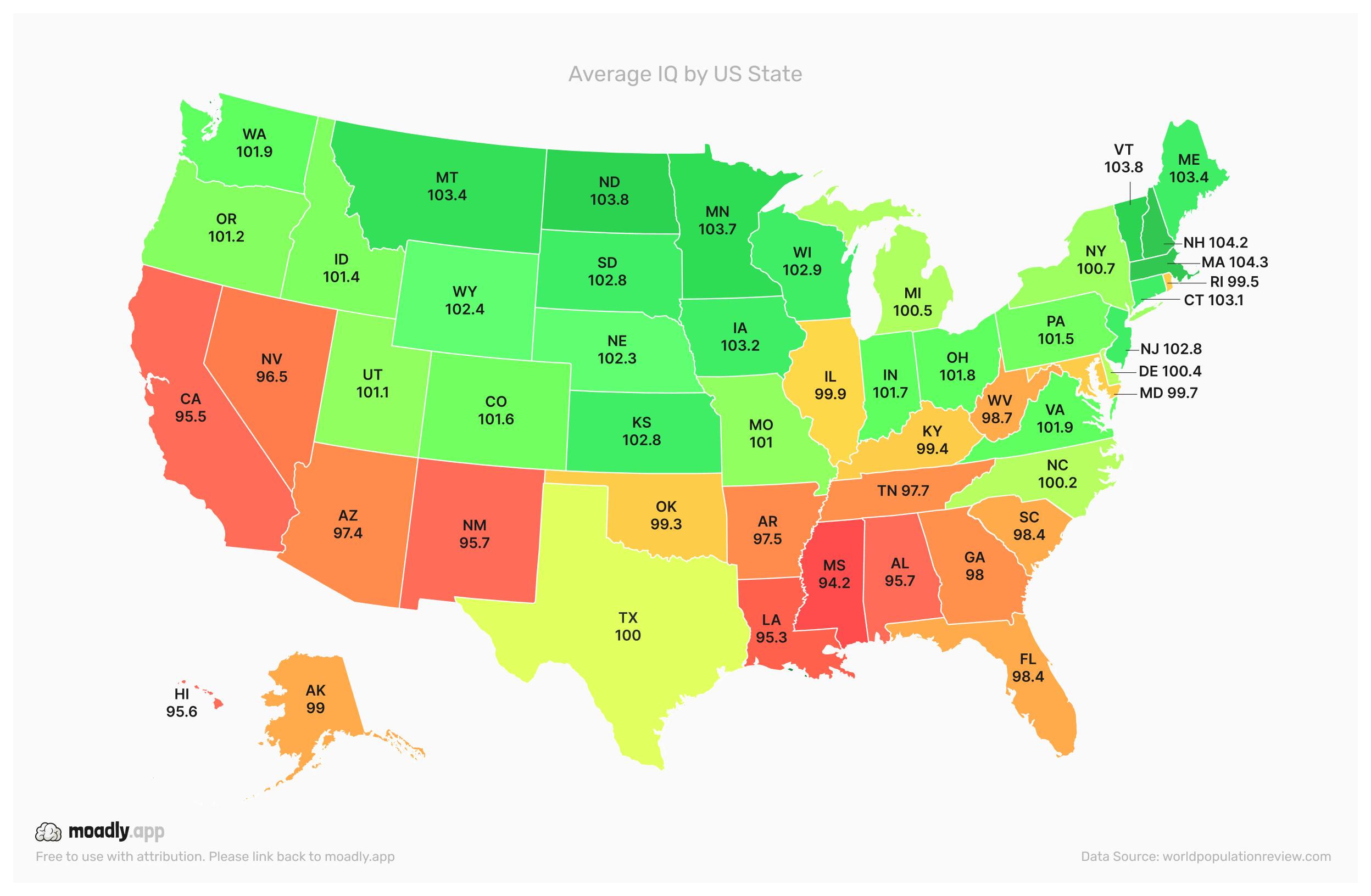
Understanding the relationship between average IQ and Subjective Cognitive Decline (SCD) can provide valuable insights into cognitive health across the U.S. While IQ reflects general cognitive ability, SCD measures self-reported memory and thinking concerns. These two indicators capture different aspects of brain function-one objective, the other subjective-but together, they can reveal broader geographic patterns.
In general, states with higher average IQ scores tend to report lower rates of SCD. This trend likely reflects the influence of education, socioeconomic stability, and access to healthcare-all factors that support both cognitive performance and awareness of mental health.
Conversely, many states with lower average IQ scores also show higher SCD prevalence, suggesting potential links between lifelong cognitive development, environmental stressors, and self-perceived cognitive decline later in life.
However, these patterns are not universal, and some states deviate from this trend.
It’s important to note that IQ and SCD are not direct measures of one another, and correlation does not imply causation.
Still, comparing these datasets provides useful context for understanding how cognitive health varies geographically and may help identify populations that could benefit from targeted prevention, education, and early intervention strategies.
| State | Average IQ | SCD Prevalence (%) |
|---|---|---|
| Massachusetts | 104.3 | 9.3 |
| New Hampshire | 104.2 | 8.9 |
| North Dakota | 103.8 | 9.9 |
| Vermont | 103.8 | 9.8 |
| Minnesota | 103.7 | 12.5 |
| Maine | 103.4 | 10.3 |
| Montana | 103.4 | 9.8 |
| Iowa | 103.2 | 9.3 |
| Connecticut | 103.1 | 7.3 |
| Wisconsin | 102.9 | 10.9 |
| Kansas | 102.8 | 0.1 |
| New Jersey | 102.8 | 9.7 |
| South Dakota | 102.8 | 6 |
| Wyoming | 102.4 | 11.2 |
| Nebraska | 102.3 | 9.4 |
| Virginia | 101.9 | 8.9 |
| Washington | 101.9 | 11.1 |
| Ohio | 101.8 | 10.7 |
| Indiana | 101.7 | 10.5 |
| Colorado | 101.6 | 10.8 |
| Pennsylvania | 101.5 | - |
| Idaho | 101.4 | 10.8 |
| Oregon | 101.2 | 11.1 |
| Utah | 101.1 | 10.7 |
| Missouri | 101.0 | 10.4 |
| New York | 100.7 | 11.2 |
| Michigan | 100.5 | 12 |
| Delaware | 100.4 | 8.8 |
| North Carolina | 100.2 | 10.7 |
| Texas | 100.0 | 13.1 |
| Illinois | 99.9 | 9.6 |
| Maryland | 99.7 | 8.6 |
| Rhode Island | 99.5 | 11.5 |
| Kentucky | 99.4 | 12.1 |
| Oklahoma | 99.3 | 13.6 |
| Alaska | 99.0 | 11.3 |
| West Virginia | 98.7 | 10 |
| Florida | 98.4 | 11.3 |
| South Carolina | 98.4 | 12.1 |
| Georgia | 98.0 | 11.2 |
| Tennessee | 97.7 | 12.1 |
| Arkansas | 97.5 | 16.2 |
| Arizona | 97.4 | 13.4 |
| Nevada | 96.5 | 16.3 |
| Alabama | 95.7 | 12.9 |
| New Mexico | 95.7 | 12.5 |
| Hawaii | 95.6 | 8.5 |
| California | 95.5 | 11.7 |
| Louisiana | 95.3 | 14.6 |
| Mississippi | 94.2 | 15.2 |
| United States (average) | 100.3 | 11.1 |
Conclusion
Analyzing SCD and average IQ across U.S. states reveals clear geographic differences in cognitive health. Some states consistently report higher cognitive performance and lower memory complaints, while others face elevated SCD and lower IQ scores. These patterns highlight how education, healthcare access, and socioeconomic factors influence both objective and subjective cognitive function.
Understanding these disparities is critical for public health planning. Policymakers and healthcare providers can use this information to prioritize early interventions, allocate resources effectively, and implement programs that support cognitive health in states with higher SCD prevalence.
For individuals, these findings underscore the importance of proactive brain health strategies. Engaging in cognitive exercises, maintaining a healthy lifestyle, and seeking regular medical guidance can help reduce the risk or impact of cognitive decline.
Ultimately, combining insights from SCD data and IQ mapping offers a comprehensive view of cognitive wellness across the country. By translating these insights into targeted actions, communities can better support older adults, improve quality of life, and reduce the long-term effects of cognitive decline nationwide.



 Color Mode
Color Mode 




